LAS VEGAS (KLAS) — Las Vegas cases involving a fungus classified by health officials as a “superbug” spiked in March and continue to grow in hospitals and other care facilities.
Since 8 News Now reported a January spike in clinical cases that resulted in infections, state records show clinical cases have dropped. But “colonization” cases — when the fungus is found on the patient’s body but there is no infection — have increased dramatically. Clinical cases are more dangerous, but colonization cases contribute to the spread.
The Nevada Division of Public and Behavioral Health reports a total of 3,685 cases have been detected since candida auris (c. auris) was first detected here in August 2021. That total includes 1,217 clinical cases and 2,368 colonization cases.
Cases reported over the past three months (February-April) show 726 new cases — 182 clinical and 544 colonizations. Numbers for the month of May — currently 119 total, with about a third classified as clinical — are not complete.

C. auris is considered by the U.S. Centers for Disease Control and Prevention (CDC) to be one of five “superbugs” that pose urgent threats. Superbugs are strains of bacteria, viruses, parasites and fungi that are resistant to most antibiotics and medications used to treat infections.
Infections from c. auris can be deadly, but state officials have stopped reporting deaths because it’s often difficult to assign a specific cause of death. Patients who contract c. auris are often fighting other severe medical problems.
Sunrise Hospital and Medical Center continues to lead the list of Nevada acute care hospitals in numbers of cases reported with a total of 1,020 since 2021 (428 clinical, 592 colonization). That’s about 27% of the cases statewide, and represents an increase since November 2023, when cases at Sunrise were 22% of the Nevada total.
Next on the list is Valley Hospital Medical Center, with 388 (144 clinical, 244 colonization). Spring Valley Hospital has the third highest total among Las Vegas hospitals with 236 (52 clinical, 184 colonization).
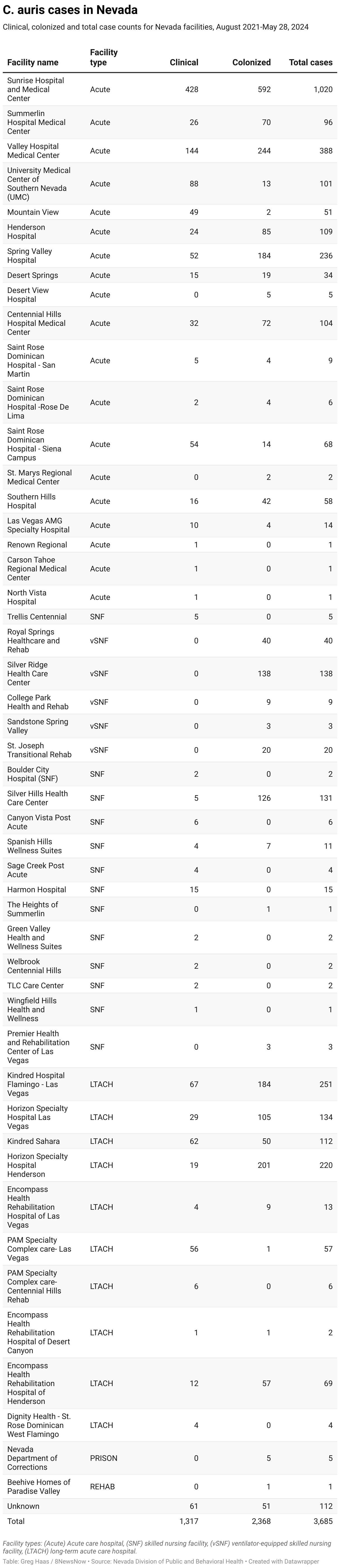
From there, a pair of long-term acute care facilities fill out the top 5. Kindred Hospital Flamingo – Las Vegas is fourth with 251 cases since 2021 (67 clinical, 184 colonization), and Horizon Specialty Hospital Henderson is fifth at 220 cases (19 clinical, 201 colonization).
The county hospital, University Medical Center of Southern Nevada, reports 101 cases (88 clinical, 13 colonization).
While no one want to be at the top of the list, Dr. Steven Merta, chief medical officer at Sunrise, said it’s expected at a hospital that handles the most at-risk patients. Sunrise is the largest acute care hospital in the state with 834 beds. Patients from all over the state, and even a big chunk of western Arizona, are frequently sent to Sunrise.
The CDC was onsite at the hospital for a week in May of 2022, and Sunrise has been documenting cases since. Merta described dealing with c. auris as “a journey” during a Friday interview.
“We have the most critically ill patients, we have those that are immunocompromised. We have those that have burns and wounds. So to have higher numbers of both clinical and colonization absolutely does not surprise us,” Merta said. “Our goal is to identify you, protect you, treat you and make sure that we are at the forefront of preventing the spread of c. auris in our facility and our community.”
Foremost, Merta emphasizes that people shouldn’t worry about coming to the hospital.
“Know that we go above and beyond the normal CDC recommendations in terminal cleaning with our advanced purification systems. So our goal is to be here for you, our community. If you need us, do not hesitate to come to the facility, come to Sunrise,” he said.
Merta said Sunrise tests more people for the fungus than other acute care hospitals. And if you don’t test, you might not know it’s there.
“We are screening many, many patients so that we can identify them, isolate them, appropriately care for them and protect everyone else in our facility,” he said.
It’s routine for the hospital to screen:
- burn patients
- patients with wounds
- patients coming from other post-acute care facilities
- patients from shelters or otherwise experiencing homelessness
And while catheters have been identified as a potential way for c. auris to cause an invasive infection, Merta said Sunrise has identifies wounds as a bigger risk.
“Catheters are only a small portion of it. Where we see the greatest risk to the patients in our community, are those with wounds, open wounds. Similar, if you think about MRSA (methicillin-resistant Staphylococcus aureus) how it was 20 years ago,” he said.





